Diabetes is a chronic disease that occurs when the pancreas is no longer able to make insulin, or when the body cannot make good use of the insulin it produces. Not being able to produce insulin or use it effectively, leads to raised glucose levels in the blood (known as hyperglycaemia). Over the long-term high glucose levels are associated with damage to the body and failure of various organs and tissues. There are over 240,000 people in New Zealand who have been diagnosed with diabetes (about 6% of the total population).
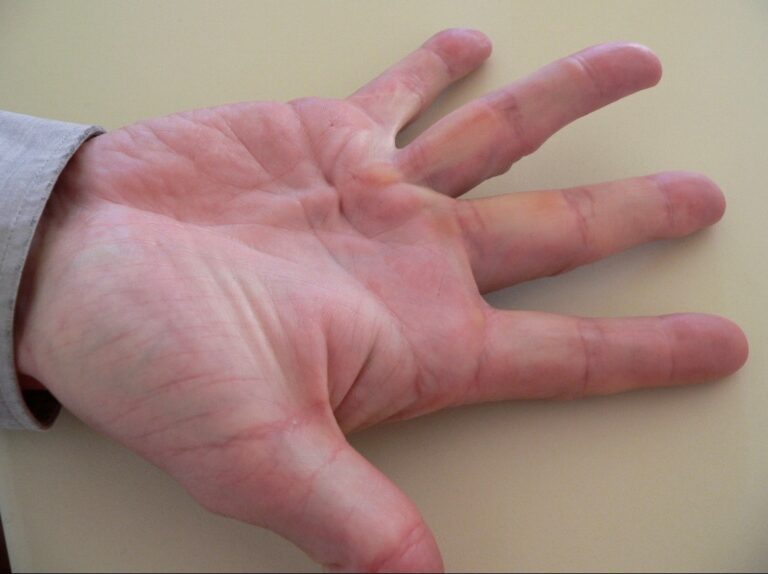
Diabetics are more susceptible to developing trigger finger. A trigger finger can be stiff and painful with gripping. Later, the finger may lock when bent and click when straightening. Symptoms are often worse in the morning. There may also be a tender nodule (or lump) felt at the top of the palm.
Incidence of trigger finger in the general population is between 2% and 3%, compared with 10% in the diabetic population. Older adults and those who have had diabetes for many years are the most likely to develop diabetic trigger finger.
There are few differences in presentation between nondiabetic and diabetic trigger finger. Diabetic trigger finger is more common in women than nondiabetic trigger finger. Trigger finger in diabetics is also more likely to present in both hands and in multiple digits.
The cause or reason for developing diabetic trigger finger remains unclear. It is thought that chronic hyperglycaemia (when the blood glucose level is too high because the body isn’t properly using or doesn’t make the hormone insulin) creates cross-links between collagen molecules and this results in collagen build-up in the tendon sheaths around the flexor tendons. The duration of diabetes, age of the patient, and glucose control are thought to affect the severity of symptoms, therefore strict glucose control is a necessary component of treatment.
Non-Surgical Treatment
Patients with minimal symptoms may try non-invasive treatments first. These may include an oral anti-inflammatories, massage and a splint to prevent the triggering. The success of these non-invasive treatments depends on the severity of the trigger finger. Often people with more painful symptoms have passed the point when simple steps are helpful. That said, a trial of simple treatments is certainly reasonable.
The next level of treatment for trigger finger includes corticosteroid injections. It is estimated that corticosteroid injections are an effective treatment for 50% to 70% of people with trigger finger. However, these injections are generally less effective in people with certain underlying health conditions, such as diabetes and rheumatoid arthritis.
Surgical treatment
Research has shown that 20% to 50% of patients with trigger finger, eventually require surgical management and diabetics make up the larger percentage. Complete release of the A1 pulley may be necessary to prevent continuation of symptoms and recurrence. This is a simple procedure that takes approximately 20 minutes and has a high success rate.
Hand therapy rehabilitation following surgery may include scar management, restoration of full finger movement and a graduated exercise programme to restore grip and pinch strength.