Carpal tunnel syndrome is a common nerve compression condition estimated to affect between 3 – 6% of the population. It may be up to three times more common in woman than men with the highest prevalence of this condition seen in the 45 – 55 year old age group.
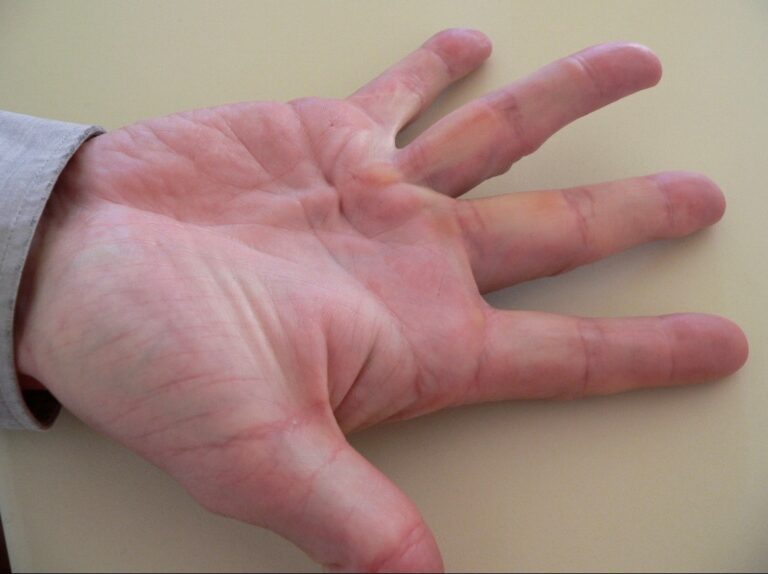
Carpal tunnel syndrome is caused by pressure on the median nerve as it passes through a narrow tunnel in the wrist. When the median nerve has pressure placed on it, patients may experience symptoms that include tingling, pins and needles and/or numbness in the thumb, index or middle finger. In more severe cases the hand feels weak and clumsy. Symptoms are often most noticeable at night time, or when performing specific activities e.g. driving.
Mild to moderate carpal tunnel symptoms often respond well to conservative management including night splinting, activity modification and nerve gliding exercises. If symptoms do not improve with treatment, or in cases of severe nerve compromise (permanent numbness and/or muscle wasting) a procedure called a carpal tunnel release (to reduce pressure on the nerve) is performed by a surgeon. Carpal tunnel release surgery is a low-risk procedure with a high level of success in relieving night time and neurological symptoms.
Recovery timelines can vary widely for those who have a carpal tunnel surgery. Factors that can influence the rate of recovery include:
- Patient age and other health factors
- The severity of carpal tunnel syndrome prior to surgery
- The ability of the patient to follow post-surgical care guidelines
Recovery Milestones
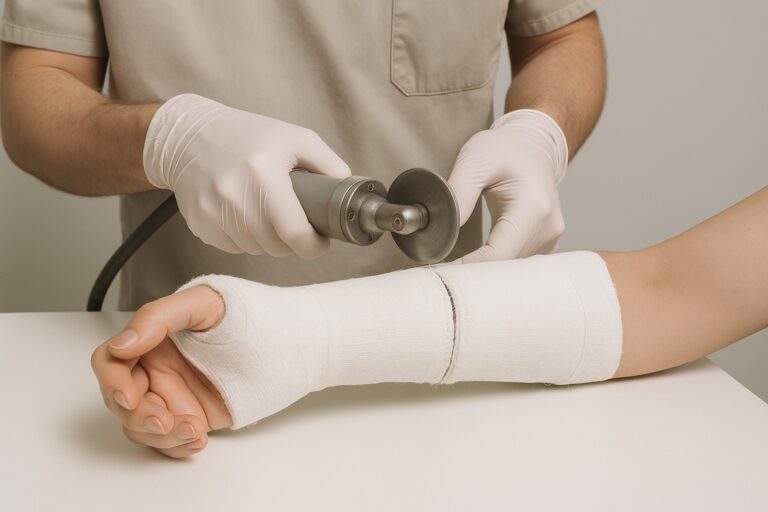
Week 1: The bandage and stitches are removed. Patients are referred to hand therapy to reduce stiffness and restore range of motion.
Weeks 2-4: Patients gradually resume activity in the affected hand. Return to work is based on the type of work required and patients with sedentary or desk jobs that don’t require heavy lifting or labour can often return to work. Patients can expect pain in the palm of the hand and soreness to touch to gradually decrease. Massaging the scar with cream helps decrease this discomfort and softens the area of the scar. Silicone tapes applied over the area of the scar are also helpful in scar management.
Driving, self-care activities, typing, and light lifting and gripping are permitted around this time. A splint may be used occasionally during this time to take pressure off the wrist and alleviate pain.
Week 4: Patients should regain full mobility of the digits in the hand by this time. If progress is slow rehabilitation should include working with a hand therapist to regain mobility.
Weeks 6-8: Patients should be close to returning to normal daily life and sporting activities but will still feel some soreness in the palm to deep pressure or touch. Night time symptoms will have improved, but there may still be some numbness in the fingers.
1 year: By this point most patients will have received all the benefits of their carpal tunnel release surgery. Patients who had severe or chronic median nerve damage, pinched nerves in the neck, or wasting of muscles prior to surgery may continue to have limits in hand function and strength even after surgery. Numbness, coordination and strength in the hand gradually improves over several weeks and months and may improve up to or beyond a year from the surgery.
If you have concerns that you may be experiencing carpal tunnel syndrome symptoms, contact a registered hand therapist for help and advice.